A promising step forward for predicting lung cancer
Over the past three years, teams at Google have been applying AI to problems in healthcare—from diagnosing eye disease to predicting patient outcomes in medical records. Today we’re sharing new research showing how AI can predict lung cancer in ways that could boost the chances of survival for many people at risk around the world.
Lung cancer results in over 1.7 million deaths per year, making it the deadliest of all cancers worldwide—more than breast, prostate, and colorectal cancers combined—and it’s the sixth most common cause of death globally, according to the World Health Organization. While lung cancer has one of the worst survival rates among all cancers, interventions are much more successful when the cancer is caught early. Unfortunately, the statistics are sobering because the overwhelming majority of cancers are not caught until later stages.
Over the last three decades, doctors have explored ways to screen people at high-risk for lung cancer. Though lower dose CT screening has been proven to reduce mortality, there are still challenges that lead to unclear diagnosis, subsequent unnecessary procedures, financial costs, and more.
Our latest research
In late 2017, we began exploring how we could address some of these challenges using AI. Using advances in 3D volumetric modeling alongside datasets from our partners (including Northwestern University), we’ve made progress in modeling lung cancer prediction as well as laying the groundwork for future clinical testing. Today we’re publishing our promising findings in “Nature Medicine.”
Radiologists typically look through hundreds of 2D images within a single CT scan and cancer can be miniscule and hard to spot. We created a model that can not only generate the overall lung cancer malignancy prediction (viewed in 3D volume) but also identify subtle malignant tissue in the lungs (lung nodules). The model can also factor in information from previous scans, useful in predicting lung cancer risk because the growth rate of suspicious lung nodules can be indicative of malignancy.

This is a high level modeling framework. For each patient, the AI uses the current CT scan and, if available, a previous CT scan as input. The model outputs an overall malignancy prediction.
In our research, we leveraged 45,856 de-identified chest CT screening cases (some in which cancer was found) from NIH’s research dataset from the National Lung Screening Trial study and Northwestern University. We validated the results with a second dataset and also compared our results against 6 U.S. board-certified radiologists.
When using a single CT scan for diagnosis, our model performed on par or better than the six radiologists. We detected five percent more cancer cases while reducing false-positive exams by more than 11 percent compared to unassisted radiologists in our study. Our approach achieved an AUC of 94.4 percent (AUC is a common common metric used in machine learning and provides an aggregate measure for classification performance).
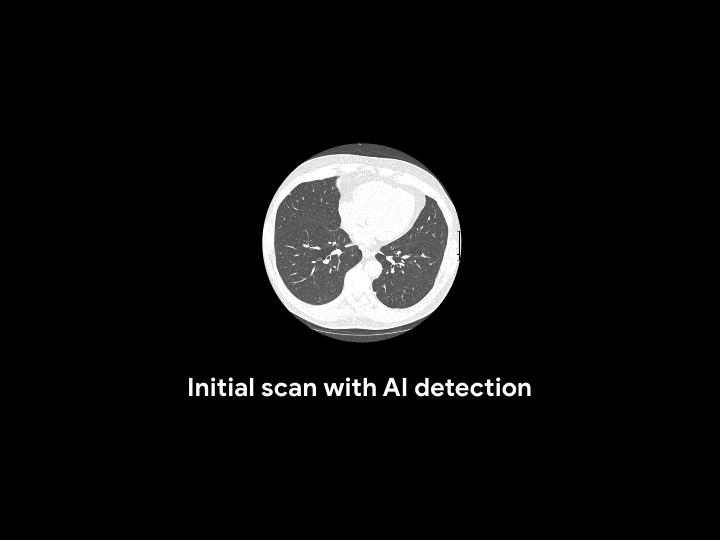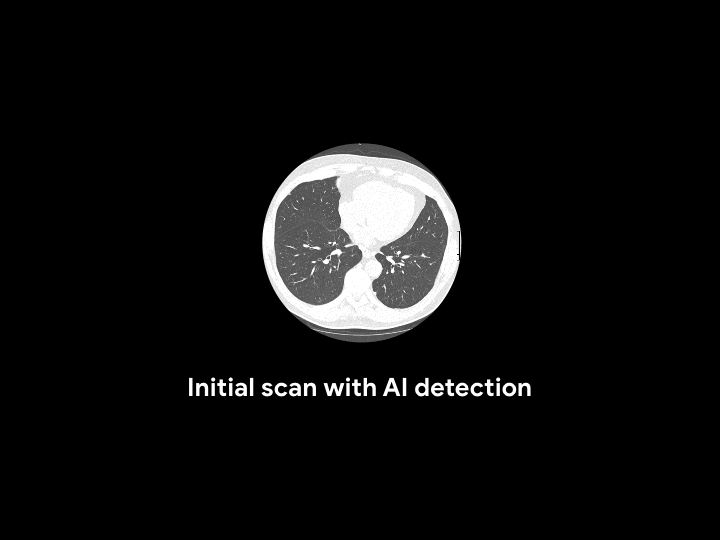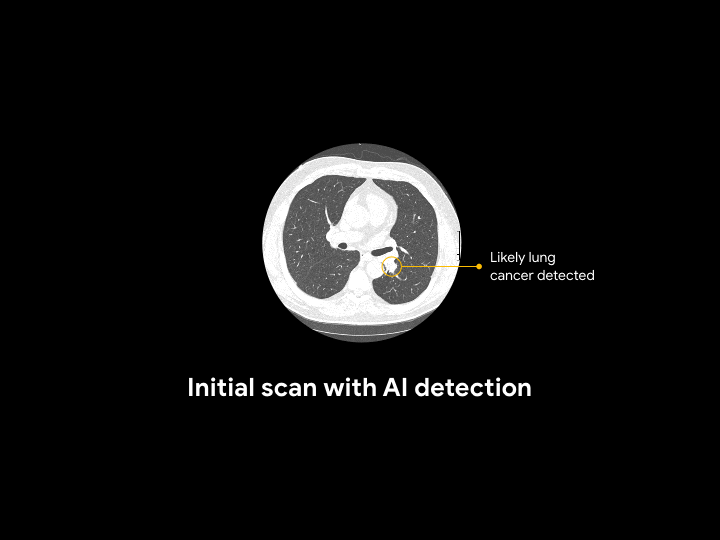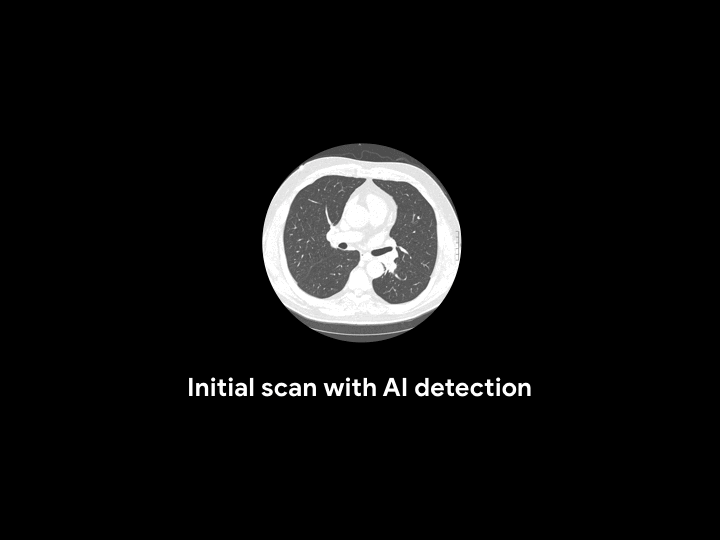
For an asymptomatic patient with no history of cancer, the AI system reviewed and detected potential lung cancer that had been previously called normal.
Next steps
Despite the value of lung cancer screenings, only 2-4 percent of eligible patients in the U.S. are screened today. This work demonstrates the potential for AI to increase both accuracy and consistency, which could help accelerate adoption of lung cancer screening worldwide.
These initial results are encouraging, but further studies will assess the impact and utility in clinical practice. We’re collaborating with Google Cloud Healthcare and Life Sciences team to serve this model through the Cloud Healthcare API and are in early conversations with partners around the world to continue additional clinical validation research and deployment. If you’re a research institution or hospital system that is interested in collaborating in future research, please fill out this form.